Have you ever walked into a room and felt an immediate sense of unease without knowing why? Or perhaps you’ve experienced a sudden wave of anxiety right after a heavy meal. For years, we were told to ignore these physical sensations or dismiss them as simple indigestion. But what if your gut is actually trying to communicate something far more significant than just hunger?
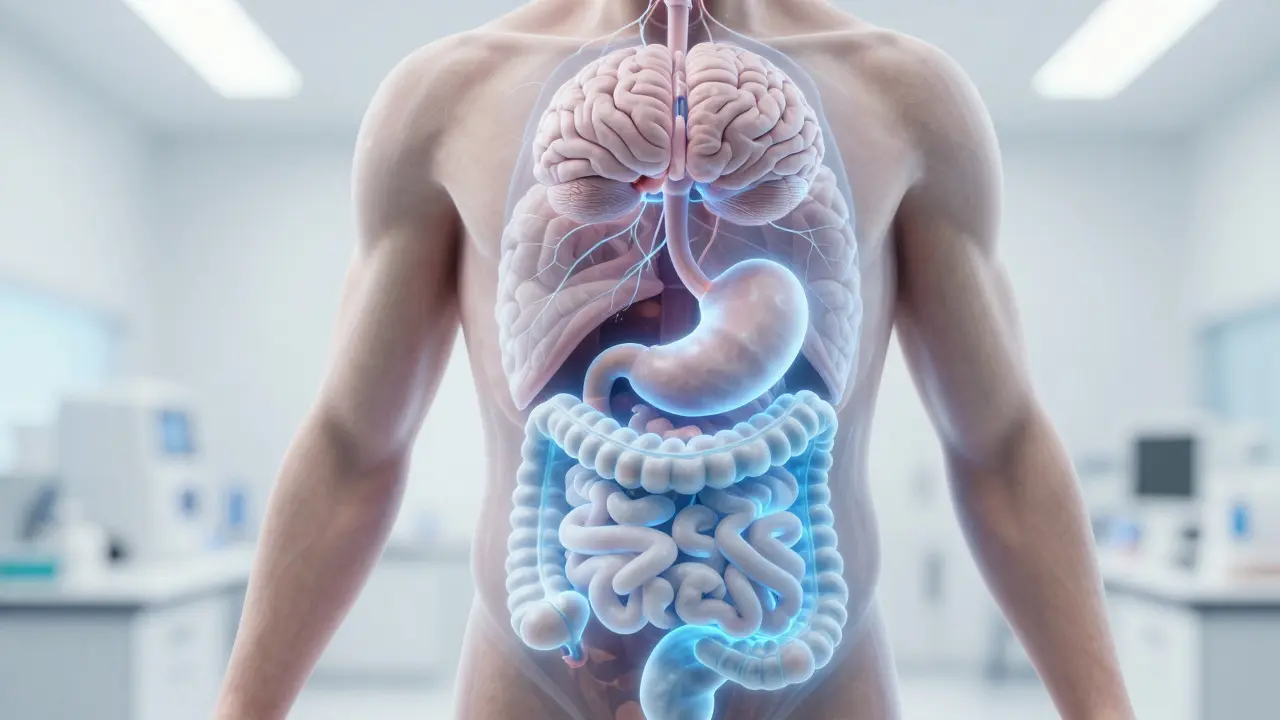
The concept of Gastro Health, often referred to as gut health, is not just about avoiding stomach aches. It is the foundation of your entire well-being, influencing everything from your mood to your immune response. When people talk about the "second brain," they aren't using poetic language; they are referring to the complex network of neurons that lines your digestive tract.
The Second Brain: Understanding the Enteric Nervous System
Your digestive system contains over 100 million neurons. This collection of nerves is known as the Enteric Nervous System (ENS). Unlike the rest of your nervous system, which requires signals from your brain to function, the ENS can operate independently. It manages digestion, nutrient absorption, and waste elimination without you having to think about it.
This independence is crucial. If your gut relied solely on your central brain for every digestive task, you would be mentally exhausted by noon. However, the connection between the two is bidirectional. The ENS communicates with the brain via the Vagus Nerve. This nerve acts as a superhighway, sending signals back and forth. When your gut is inflamed or irritated, it sends distress signals up the Vagus Nerve, which your brain interprets as stress, anxiety, or even depression.
Consider this scenario: You have a big presentation at work. Your stomach starts churning. That isn't just nerves; it's your gut reacting to cortisol, the stress hormone. Conversely, if your gut is full of unhealthy bacteria due to poor diet, it can send constant low-level stress signals to your brain, making you feel anxious even when nothing is wrong. This explains why improving gastro health often leads to better emotional stability.
The Microbiome: A Ecosystem Within You
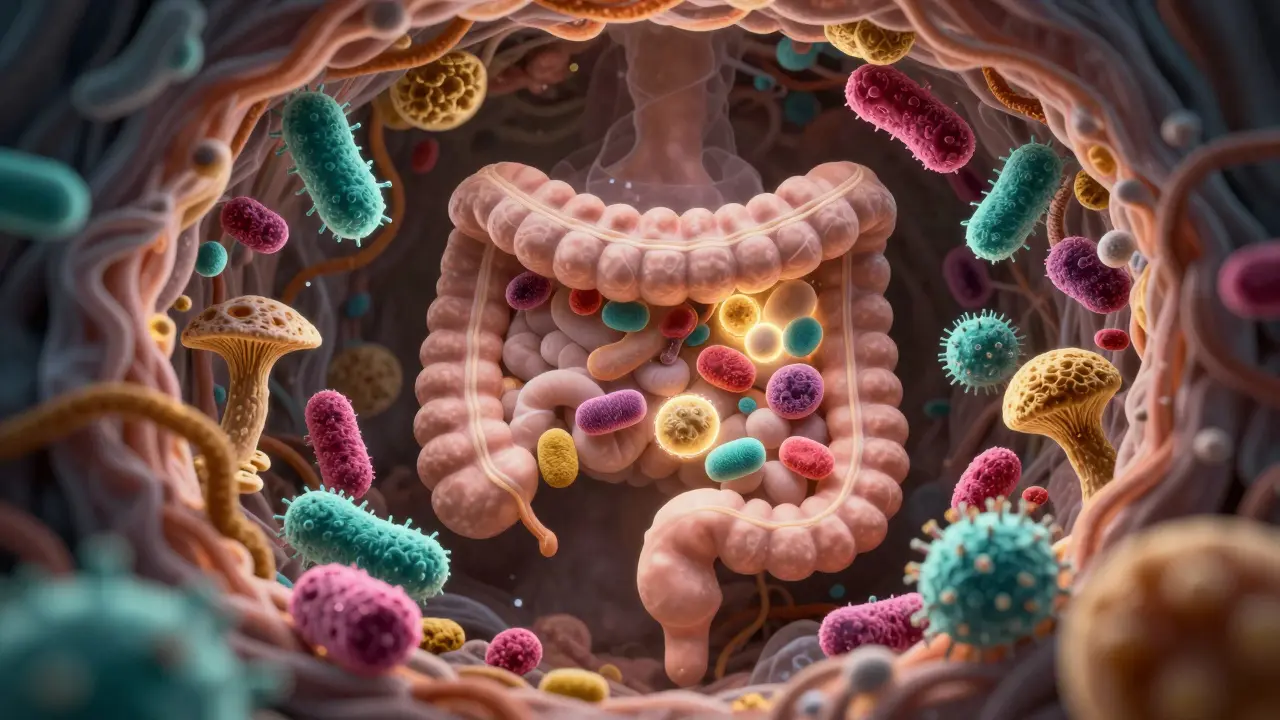
Inside your intestines lives a vast community of microorganisms. Scientists call this the Microbiome. It consists of trillions of bacteria, viruses, fungi, and other microbes. While "germs" usually sound bad, these specific microbes are essential for life. They outnumber your human cells and play a critical role in breaking down food, synthesizing vitamins, and protecting against pathogens.
A healthy microbiome is diverse. Think of it like a rainforest. A rainforest with many different species of plants and animals is resilient against disease and climate change. Similarly, a gut with a wide variety of bacterial strains is better at resisting infections and maintaining balance. When diversity drops-often due to antibiotic use, processed foods, or chronic stress-the ecosystem becomes fragile. Harmful bacteria can take over, leading to inflammation and various health issues.
Research published in journals like *Nature* has shown that individuals with inflammatory bowel diseases often have significantly lower microbial diversity compared to healthy controls. This isn't just correlation; the lack of certain beneficial bacteria directly contributes to the inflammation that damages the intestinal lining.
Gut Health and Immunity: The First Line of Defense
About 70% of your immune system resides in your gut. Specifically, it’s located in the Gut-Associated Lymphoid Tissue (GALT). This tissue trains your immune cells to distinguish between friendly nutrients and harmful invaders. When your gastro health is compromised, this training process goes awry.
If the barrier between your gut and bloodstream becomes leaky-a condition known as "leaky gut" or increased intestinal permeability-undigested food particles and toxins can enter the bloodstream. Your immune system sees these foreign substances and launches an attack. This systemic inflammation is linked to a host of chronic conditions, including autoimmune diseases, allergies, and even skin conditions like eczema and acne.
For example, studies suggest a strong link between gut dysbiosis (an imbalance of gut bacteria) and rheumatoid arthritis. By restoring balance to the microbiome, some patients see a reduction in joint pain and swelling. This highlights that treating the gut might be more effective than treating the symptoms elsewhere in the body.
| Feature | Prebiotics | Probiotics |
|---|---|---|
| Definition | Fiber that feeds good bacteria | Live beneficial bacteria |
| Sources | Garlic, onions, bananas, oats | Yogurt, kefir, sauerkraut, kimchi |
| Function | Promotes growth of existing good bacteria | Adds new beneficial strains to the gut |
| Survival | Resists digestion to reach colon | Must survive stomach acid to be effective |
Nourishing Your Gut: Diet and Lifestyle Choices
You cannot buy your way to perfect gut health with supplements alone. The most powerful tool you have is your daily diet. To support your microbiome, you need to feed the good bacteria. This means eating plenty of Prebiotic fibers. These are types of carbohydrates that your body cannot digest but that serve as food for beneficial bacteria.
Incorporate foods like garlic, onions, leeks, asparagus, and bananas into your meals. Whole grains like oats and barley also provide excellent prebiotic fuel. In Australia, native ingredients like finger limes and wattleseed are gaining popularity not just for their unique flavors but for their high fiber content, which supports digestive regularity.
Alongside prebiotics, Probiotics introduce live cultures to your gut. Fermented foods are the best source. Sauerkraut, kimchi, miso, and kefir are packed with diverse bacterial strains. Unlike pills, fermented foods contain the bacteria in their natural matrix, along with enzymes and other compounds that aid digestion. Try adding a small serving of fermented vegetables to lunch or dinner daily.
However, what you avoid is just as important as what you eat. Ultra-processed foods, artificial sweeteners, and excessive alcohol can disrupt the microbiome. Emulsifiers found in packaged snacks, for instance, have been shown to thin the mucus layer of the gut, making it easier for harmful bacteria to cause inflammation. Reading labels and choosing whole, unprocessed foods is one of the simplest steps you can take.
The Stress-Gut Connection
We often treat stress and digestion as separate issues, but they are deeply intertwined. Chronic stress alters the composition of your gut bacteria. High levels of cortisol reduce blood flow to the digestive organs, slowing down digestion and allowing harmful bacteria to thrive. This creates a vicious cycle: stress harms the gut, and a harmed gut increases stress sensitivity.
To break this cycle, practices that activate the parasympathetic nervous system-the "rest and digest" mode-are essential. Deep breathing exercises, mindfulness meditation, and adequate sleep can help calm the Vagus Nerve. Even a short walk in nature, away from screens and city noise, can lower cortisol levels and improve gut motility. In Brisbane, taking advantage of the local parks and green spaces offers a practical way to integrate this into your routine.

Signs Your Gut Needs Attention
Your body gives you clues when your gastro health is off track. Persistent bloating, gas, and irregular bowel movements are obvious signs. But look deeper. Do you experience frequent heartburn or acid reflux? Do you suffer from unexplained fatigue or brain fog? Are you prone to food sensitivities that didn't exist before?
Skin issues like eczema, psoriasis, or persistent acne can also stem from gut inflammation. If you find yourself constantly battling minor infections or feeling run-down despite getting enough sleep, your immune system may be struggling due to a compromised gut barrier. Recognizing these early warning signs allows you to address the root cause rather than just masking symptoms with medication.
Moving Forward: Practical Steps for Better Gastro Health
Improving your gut health doesn't require a drastic overhaul overnight. Start small. Add one new vegetable to your dinner each day. Swap out sugary drinks for water or herbal tea. Introduce one fermented food into your weekly routine. Listen to your body. If certain foods make you feel sluggish or bloated, try eliminating them for a few weeks and observe the difference.
Remember, consistency is key. The microbiome responds to long-term habits, not quick fixes. By prioritizing your gastro health, you invest in your energy, mood, immunity, and longevity. It is truly more important than you think, acting as the silent guardian of your overall well-being.
What are the first signs of poor gut health?
Common signs include persistent bloating, gas, constipation, diarrhea, acid reflux, and unexplained fatigue. Skin issues like eczema and frequent food sensitivities can also indicate underlying gut inflammation.
How does gut health affect mental health?
The gut and brain communicate via the Vagus Nerve. An unhealthy microbiome can send stress signals to the brain, contributing to anxiety and depression. Conversely, a balanced gut produces neurotransmitters like serotonin, which regulate mood.
What foods are best for healing the gut?
Focus on prebiotic-rich foods like garlic, onions, bananas, and oats to feed good bacteria. Include probiotic-rich fermented foods such as yogurt, kefir, sauerkraut, and kimchi to introduce beneficial microbes. Avoid ultra-processed foods and excessive sugar.
Can stress damage your digestive system?
Yes. Chronic stress releases cortisol, which reduces blood flow to the gut and alters the microbiome composition. This can lead to slower digestion, inflammation, and increased susceptibility to digestive disorders.
How long does it take to improve gut health?
While some improvements in digestion can be noticed within days of dietary changes, fully restoring a diverse and resilient microbiome typically takes several weeks to months of consistent healthy eating and lifestyle habits.